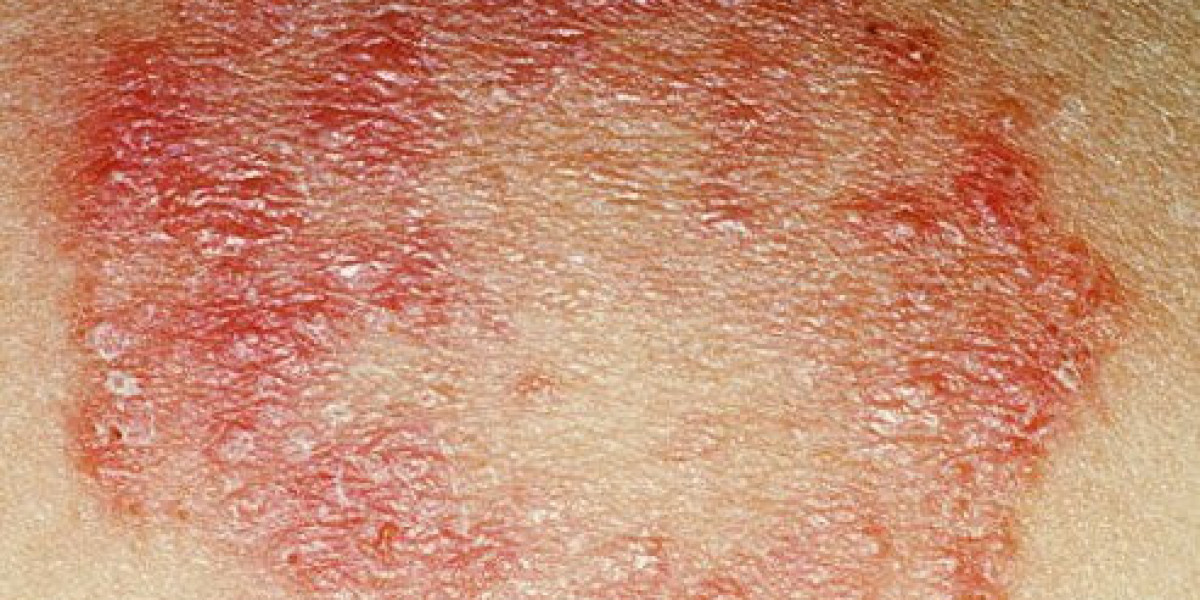
Bacterial skin infections are common clinical conditions that range from mild, superficial involvement to deeper, potentially systemic disease. Prompt recognition and early intervention are essential to prevent complications such as abscess formation, cellulitis spread, or systemic bacteremia. This guide outlines practical, evidence-based quick fixes for bacterial skin infections while addressing antibiotic access considerations, including sourcing options such as cephalexin capsules wholesale for healthcare providers and pharmacies.
Understanding Bacterial Skin Infections
Bacterial skin infections typically occur when pathogenic organisms breach the protective barrier of the epidermis. The most common causative organisms are Staphylococcus aureus (including MRSA strains) and Streptococcus pyogenes.
Common clinical presentations include
Impetigo – superficial crusted lesions, often honey-colored
Folliculitis – inflamed hair follicles
Furuncles and carbuncles – deeper follicular infections
Cellulitis – diffuse, spreading inflammation of dermis and subcutaneous tissue
Erysipelas – sharply demarcated superficial cellulitis
Each condition requires slightly different management, but early treatment principles remain consistent.
Quick Fix #1: Early Cleansing and Topical Care
For mild and superficial infections:
Clean the area with mild soap and warm water twice daily.
Apply topical antiseptics such as chlorhexidine or povidone-iodine.
Use topical antibiotics (e.g., mupirocin) when impetigo is localized.
Keeping the affected area dry and covered reduces bacterial spread and autoinoculation.
This conservative approach may resolve minor infections within 5–7 days without systemic antibiotics.
Quick Fix #2: Warm Compresses for Localized Abscesses
For small boils or early abscess formation:
Apply warm compresses 3-4 times daily.
This increases local blood flow.
It promotes spontaneous drainage.
However, abscesses larger than 1-2 cm typically require incision and drainage by a healthcare professional.
Quick Fix #3: Oral Antibiotics for Moderate Infections
When infection extends beyond superficial layers or shows spreading erythema, systemic therapy becomes necessary. One of the most commonly prescribed first-line oral antibiotics is cephalexin, a first-generation cephalosporin effective against many gram-positive organisms.
Why Cephalexin?
Strong coverage for Streptococcus species
Effective against methicillin-sensitive Staphylococcus aureus (MSSA)
Well tolerated
Favorable safety profile
Affordable and widely available
Cephalexin is often indicated in cases of:
Mild to moderate cellulitis
Infected wounds
Post-surgical site infections
Non-MRSA skin infections
Standard adult dosing typically ranges from 250 mg to 500 mg every 6 hours, depending on severity. Treatment duration is usually 5–10 days.
Access and Supply Considerations
Healthcare facilities, urgent care centers, and pharmacies must maintain consistent antibiotic supply chains. Bulk procurement strategies, such as sourcing cephalexin capsules wholesale, can:
Reduce per-unit medication costs
Ensure adequate stock during seasonal spikes
Improve dispensing efficiency
Maintain treatment continuity
Wholesale purchasing is especially critical for community clinics and telehealth providers who treat high volumes of uncomplicated skin infections.
Quick Fix #4: Recognizing When MRSA Coverage Is Needed
Cephalexin does not reliably cover community-acquired MRSA. Signs that may suggest MRSA involvement include:
Rapidly progressing abscess formation
History of MRSA colonization
Recurrent infections
Poor response to beta-lactam antibiotics
In such cases, alternative antibiotics (e.g., trimethoprim-sulfamethoxazole or doxycycline) may be required. Culture and sensitivity testing should guide therapy whenever possible.
Quick Fix #5: Proper Wound Care
Open wounds serve as entry points for bacterial invasion. Effective wound management includes:
Debridement of necrotic tissue
Saline irrigation
Sterile dressing application
Daily inspection for spreading erythema
Patients should be instructed to monitor for warning signs:
Fever
Increasing redness
Streaking
Swelling
Severe pain
Escalation to emergency care is necessary if systemic symptoms develop.
Quick Fix #6: Address Underlying Risk Factors
Certain populations are predisposed to recurrent bacterial skin infections:
Diabetic patients
Immunocompromised individuals
Athletes in close-contact sports
Individuals with poor hygiene access
Managing underlying conditions improves outcomes significantly. For example:
Optimizing blood glucose levels reduces infection recurrence.
Screening for nasal Staphylococcus aureus colonization may be warranted in recurrent cases.
Quick Fix #7: Preventive Hygiene Measures
Preventing reinfection is just as important as treating active disease.
Key preventive strategies include:
Frequent hand washing
Avoiding shared personal items
Proper laundering of clothing and towels
Immediate cleansing of cuts and abrasions
Community health programs often integrate antibiotic supply management including access to cephalexin capsules wholesale with patient education initiatives to control outbreak patterns.
When to Seek Immediate Medical Attention
While many bacterial skin infections are mild, some can become life-threatening if untreated.
Emergency evaluation is required if a patient experiences:
High fever
Rapidly spreading redness
Severe pain disproportionate to appearance
Signs of necrotizing infection (e.g., skin discoloration, blisters)
Confusion or hypotension
Conditions such as necrotizing fasciitis require urgent surgical and intravenous antibiotic intervention.
Antibiotic Stewardship Considerations
Although antibiotics like cephalexin are effective, inappropriate overuse contributes to antimicrobial resistance. Clinicians should:
Confirm bacterial etiology before prescribing
Avoid treating viral or fungal skin conditions with antibiotics
Use the narrowest effective spectrum
Prescribe appropriate treatment duration
Bulk purchasing strategies such as cephalexin capsules wholesale should be paired with stewardship protocols to prevent misuse and ensure responsible distribution.
Summary
Bacterial skin infections are common but highly manageable when treated promptly. Quick fixes include:
Early cleansing and topical therapy
Warm compresses for minor abscesses
Timely initiation of oral antibiotics like cephalexin
Proper wound care
Recognition of MRSA risk
Preventive hygiene practices
For healthcare providers and pharmacies, maintaining reliable antibiotic supply chains including sourcing cephalexin capsules wholesale supports rapid treatment access and improved patient outcomes.
When addressed early, most bacterial skin infections resolve without complications. However, awareness of warning signs and adherence to proper treatment protocols remain critical for optimal recovery.